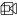Well-coordinated chains of mother banks and storage centres, supported by NGOs and altruistic donors, is the way to go

India does have a sound national blood policy, but the absence of a fully  coordinated national blood service renders a patient hapless and helpless at critical moments.
coordinated national blood service renders a patient hapless and helpless at critical moments.
In the event of a road accident or a surgical emergency, an inability on the part of patients’ relatives to organise blood may lead to a fatality. Besides, lack of access to safe blood still remains a major cause of maternal mortality in all parts of the country.

Safety of blood was ushered in an effective manner after the landmark judgment from the Supreme Court of India on January 4, 1996, which led to banning of paid blood ‘donation’ by the professional blood sellers, effective January 1, 1998.

The office of the Drugs Controller General of India and the respective Food and Drugs Control Administration department of the states are expected to closely monitor blood donation services in the country in liaison with the National and State Blood Transfusion Councils.

The National AIDS Control Organisation (NACO) and the State Blood Transfusion Councils have taken myriad steps to improve screening, processing and storage of blood for utilisation by end users. But the stark reality is that there still is a severe shortage of accessible blood with varying levels of safety. There are more than 2,000 blood banks in the country. Many of these are unregulated, with profiteering often being the main motive.

We need to have more and properly trained lab technicians, fewer but more efficient blood banks, and district-level agencies that can handle all the processes necessary to make safe blood available to the needy.
A centralised database of ‘safe’ blood donors accessible to all, say through the Websites of the State Blood Transfusion Councils can make a big difference. In most countries in the world, including many developing countries, blood services are run by the national, provincial or local self government or by organisations like the Red Cross and Red Crescent Societies.
In our country, there is an absence of a centralised management of blood services, which results in lack of standardised practices and processes, poor quality standards, inadequacy of blood availability, and a near-complete neglect of those requiring regular transfusions due to chronic disorders.
We must plan to address the issue of blood security by setting up a centralised blood collection and processing system at the mother blood banks and storage centres, on a pilot basis.
A few mother blood banks supported by organisations of voluntary donors, but run by professionals, will have to be roped in. Blood collected from voluntary blood donors will be processed using standardised and quality operating procedures at the mother blood banks. It will then be distributed to storage centres with maintenance of cold chain and stored according to standard operating procedures.
Participating hospitals will simply have to indent the required units of blood from the mother blood banks or storage centres. The existing blood banks in hospitals may function as storage and cross-matching centres.
A modern health care system cannot function effectively without a blood service that assures blood security to all. Access to safe blood must be perceived as a right of the patient.
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter, Instagram.
"Exciting news! Elets technomedia is now on WhatsApp Channels Subscribe today by clicking the link and stay updated with the latest insights!" Click here!